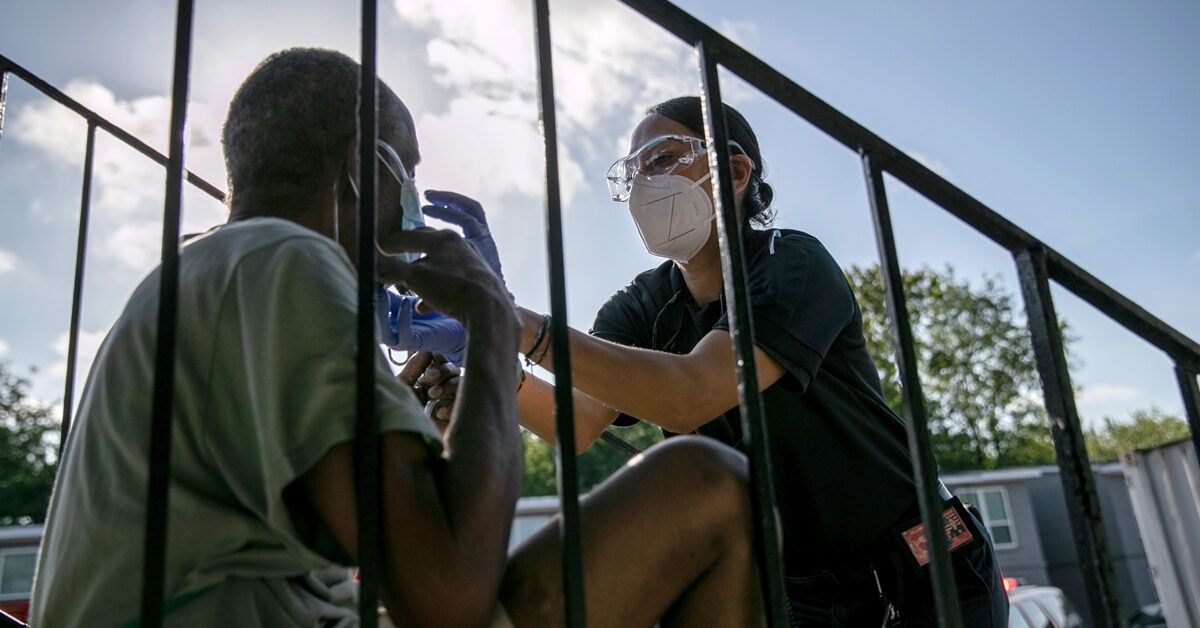
Indoor vs Outdoors - 18.7 times greater risk
A preliminary report from scientists in Japan (which has not been peer-reviewed) suggested that the odds that an infected person "transmitted COVID-19 in a closed environment was 18.7 times greater compared to an open-air environment."

 www.medrxiv.org
www.medrxiv.org
A preliminary report from scientists in Japan (which has not been peer-reviewed) suggested that the odds that an infected person "transmitted COVID-19 in a closed environment was 18.7 times greater compared to an open-air environment."

Closed environments facilitate secondary transmission of coronavirus disease 2019 (COVID-19)
Objective To identify common features of cases with novel coronavirus disease (COVID-19) so as to better understand what factors promote secondary transmission including superspreading events. Methods A total of 110 cases were examined among eleven clusters and sporadic cases, and investigated...